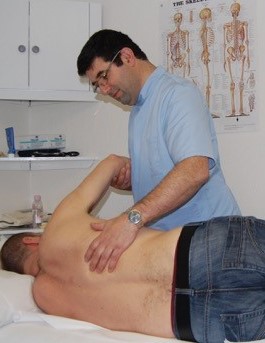
This course aims to improve the practitioners’ knowledge of the immune system and to teach enhanced palpatory skills in assessing the health of the patient’s lymphatic system. You will learn different strategies to aid lymphatic drainage in conjunction with other forms of osteopathic techniques. The course begins with a history of the lymphatic system in medicine and osteopathy. It also covers relevant anatomy, pathology and diagnosis of the lymphatic system and its disorders. Manual techniques will be demonstrated and practised.
- The anatomy of the lymphatic system from the smallest lymphatic vessel to the cisterna chyli and the thoracic duct.
- The immune system – the difference between B and T cells, the acute and chronic immune response and the significance of the relationship between the lymphatic system and the immune system.
- The physiology of the lymphatics system.
- The pathology of the lymphatics system including examination in the diagnosis of lymphatic disease.
- The neuro-lymphatic (glymphatic system) and its disorders – including the pathogenesis of Chronic Fatigue Syndrome/ Myalgic Encephalomyelitis (CFS/ME) and fibromyalgia, physical symptoms and diagnostic signs.
- Management of lymphatic disorders including contra-indications and cautions to treatment.
Summary of Osteopathic Practice Standards (Updated) and other CPD elements covered
A) Communication and patient partnership- A1, A2, A3, A4, A5, A6
B) Knowledge, skills and performance - B1, B2, B3, B4
C) Safety and quality in practice - C1, C4, C6
D) Professionalism - D2, D10
Learning Outcomes
- Understand the pathogenesis of lymphatic disorders from a biomechanical perspective.
- Learn how to examine a patient for the early physical symptoms and diagnostic signs for possible lymphadenopathies and learn the differences between healthy and non-healthy systems including splenomegaly, Hodgkin’s and fibromyalgia.
- Learn how to manage patients focussing on the lymphatics plus specific disorders such as lymphangitis, lymphoedema and other forms of lymphadenopathy.
- Gain an understanding of how to integrate the evidence-based medicine discussed in the workshop into better patient care in all realms of clinical practice.
Equipment
Delegates are requested to bring towels and oil/cream (none nut based) for effleurage techniques.
Timetable
Day 1:
09:00-09:30 Registration/Coffee
09:30-11:00 The history of lymphatic discovery, the anatomy of the lymphatic system and the immune system
11:00-11:15 Tea/Coffee break
11:15-12:30 The physiology of the lymphatics- practical session surface anatomy
12:30-13:30 Lunch
13:30-16:00 Applied Pathology: lymphatic disorders. The neurolymphatic system and disorders. Case studies: Q and A on diagnosis and clinical management of the patient. (4 real case studies will be discussed)
16:00-16:15 Tea/Coffee break
16:15-17:30 Practical training: Examination in the diagnosis of lymphatic disease; signs and symptoms, red flags, safety of the patient
Day 2:
09:30-11:00 Manual treatment of lymphatic disorders:
Based on the latest osteopathic principles and practice (Foundations of Osteopathic Medicine 4th Edition, Seffinger MA ed. AOA, 2018. Using data from osteopathic research into lymphatics supporting manual lymphatic techniques including Creasy et al 2013, Hodge et al 2010 & 2015, Huff et.al. 2010.
11:00-11:15 Tea/Coffee break
11:15-12:30 Diagnosis of neurolymphatic disorders
12:30-13:30 Lunch
13:30-16:00 Practical examination of the neuro-lymphatic system and disorders. (Hives L et al 2017)
16:00-16:15 Tea/Coffee break
16:15-17:30 Practical training: Treatment of neuro-lymphatic disease including indications and contraindications for treatment. (Perrin R et al. 1998 and 2011)
Course Suitability
The course is suitable for osteopaths, physiotherapist and chiropractors.
Recommended Pre Course Reading
The Perrin Technique, Raymond N Perrin, Hammersmith Press, London 2007.
Hives L, Bradley A, Richards J, Sutton C, Selfe J, Basu B, Maguire K, Sumner G, Gaber T, Mukherjee A, Perrin RN. Can physical assessment techniques aid diagnosis in people with chronic fatigue syndrome/myalgic encephalomyelitis? A diagnostic accuracy study. BMJ Open 2017;0:e017521. doi:10.1136/ bmjopen-2017-017521